In 2011 it was estimated that nearly 100 million Americans suffered from > 1000 neurologic disorders. If YOU have experienced numbness, parasthesias (abnormal sensations), fatigue, weakness, or pain you may be included in this staggering number. How do you know for sure? We trust we can turn to the experts for answers. But what if the answer (you are desperate to receive) is wrong? A misdiagnosis can cost you time, money, and delay treatment. So, how does this happen? And more importantly, did this happen to you? Should you accept the first diagnosis? Maybe not. Here is why….
1. Healthcare is science AND art
Many believe that healthcare is a science. In America, a trip to the pediatrician (as a young child), created this belief. Case and point. As a child, you broke your arm. An x-ray confirmed this, and the doctor fixed it. Problem solved. Science, right? Yes, advances in medicine have made broken bones, minor infections, and certain cancers a (black and white) science. However, the majority of medicine is still, very much, an art.
Art Versus Science
Some theorize that humans are either left or right brain dominant. As the theory goes, left brain dominance is more science based and right brain is more artistic. For “left brain thinkers”, you think primarily in black and white. X + Y = Z. Can you relate? On the contrary, “right brain thinkers” can see a little more gray.
An artist (known to be a “right brainer” :)) can look at a painting, or a piece of artwork, and come up with an elaborate meaning behind the art and the artist. The same artist can return for a second look and see something totally different. To a scientist (a “left brainer”), a piece of art looks like a broken vase, a painting of a naked person, or something that looks like someone fell into a canvas with a paint brush in their hand. In contrast, an artist looks deeper, analyzing the different colors, choice of paint, how the colors relate to other colors….blah blah, blah. No offense to artists, but I am 100% a “left brainer”. 🙂
The point is, healthcare is very similar. It is not ONLY about a patient’s complaints. Nor is it ONLY about a positive test, or an abnormal scan. In other words, Neurologists, known to be scientists, are also artists. They must gather all the data (patient’s complaint, diagnostic results, past medical history, family history, etc.) analyze it’s meaning, how it relates to other findings, and determine it’s value (how important it is to the big picture). In other words, Art. So, should you accept only one diagnosis? Does a painting really only have one meaning? No and…… I don’t think so. 🙂
2. Can someone PLEASE explain “abnormal” test result?
Your Radiologist or Neurologist has seen the (MRI, CT…etc.) results. And you receive the answer you have been waiting for….. “abnormal”. Seriously? Yes. Now, there are several abnormalities that can show up on an MRI. “abnormal” can have several meanings, or have no meaning at all. In other words, it could be relevant to the big picture or a benign (not harmful) anomaly. In an ideal world, an abnormal finding on an MRI initiates a thought process. It is the catalyst that propels the Neurologist toward the most appropriate next step in the evaluation process. In contrast, if a single test is used to diagnose a neurologic condition, a misdiagnosis is possible.
3. Diagnostic tests can produce a “false positive” or a misdiagnosis
Shockingly, a report released by the Institute of Medicine (IOM) in 2015 reported that 5% of adults who receive outpatient care will experience a diagnostic error. An “abnormal” finding on an MRI may be nothing more than “bad image quality”. Several factors can cause something to appear on an MRI that is NOT actually there. This could result in a false positive. For example, if a patient moves while a test is in process, the image quality may be poor. And yes, a hasty, over-booked physician may draw an inaccurate conclusion and lead to a misdiagnosis. It happens. Humans are human. And yes, this applies to doctors. 🙂
4. A differential diagnosis is critical in preventing a misdiagnosis
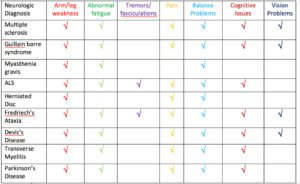
A differential diagnosis is a process of differentiating to or more conditions with similar symptoms. This is absolutely essential in diagnosing neurologic conditions. Why? Many problems in the nervous system can have similar symptoms. Here is a short list of diagnoses that share similar symptoms.
Disclaimer: This is not meant to elicit fear. Nor does this in any way mean that if you have 1 or 2 of these symptoms that you have this diagnosis. It is only meant to show the overlap that exists.
This chart illustrates several conditions that share similar symptoms and the high probability of error. Therefore, the FIRST diagnosis, might not be the correct diagnosis.
5. An accurate diagnosis requires a team, not an individual
Do to the nature of our healthcare system, a “team” of doctors, is becoming, non-existent. A hasty diagnosis has replaced the “art” of collaboration, consultations, and referrals. The present environment has forced radiologists, emergency room physicians, and internal medicine physicians into vacuum. A Neurologist’s time is occupied with immediate, life-threatening emergencies (ie: stroke, traumatic brain injury, traumatic spinal cord injury…etc). The result? Neurologist’s rely too heavily on radiologists, and other specialists for a diagnosis.
How can a physical therapist help your Neurologist and prevent a misdiagnosis?
Physical therapists are experts in the neuro-musculo-skeletal system. This is a fancy way of saying physical therapists understand nerves, muscles, and bones. A session lasts (a minimum of) one hour versus several minutes spent with a Neurologist. Therapists are trained in a patient care model that emphasizes a process:
> Listen to the patient,
> Perform a physical assessment,
> Implement treatment, and
> Re-assess to test the effectiveness of the treatment
This process does not start and stop in the first visit. This process occurs multiple times during EVERY visit. Why is this important? One, It affords the opportunity to hear a patient complaint (that might not come up during the doctor visit). Two, see an abnormal movement, or provoke a symptom (that otherwise might get missed). Finally, a physical therapist can observe the effects of a medical treatment (ie: an infusion, disease specific medication, surgical intervention…etc) in real time. This is in contrast to a patient giving a report to their Neurologist “at the next follow up visit”. This can be invaluable information to help a Neurologist rule in or rule out certain neurologic conditions and prevent a misdiagnosis.
Let’s get to the point
Ok, ok. The point is, a misdiagnosis is not really an “error”. A misdiagnosis may just be that your Neurologist was looking at you from the wrong angle (figuratively speaking), or placed emphasis on certain things and not others. There is an ancient proverb that says “measure twice, cut once”. Actually, I think it is used in carpentry, but I digress. 🙂 We use this saying everyday. It means to be thorough, and double check your work for accuracy. Do you only get one quote when building a house? Do you only look once when crossing the street? How much more important is your health. Is there any value in seeking a second opinion?